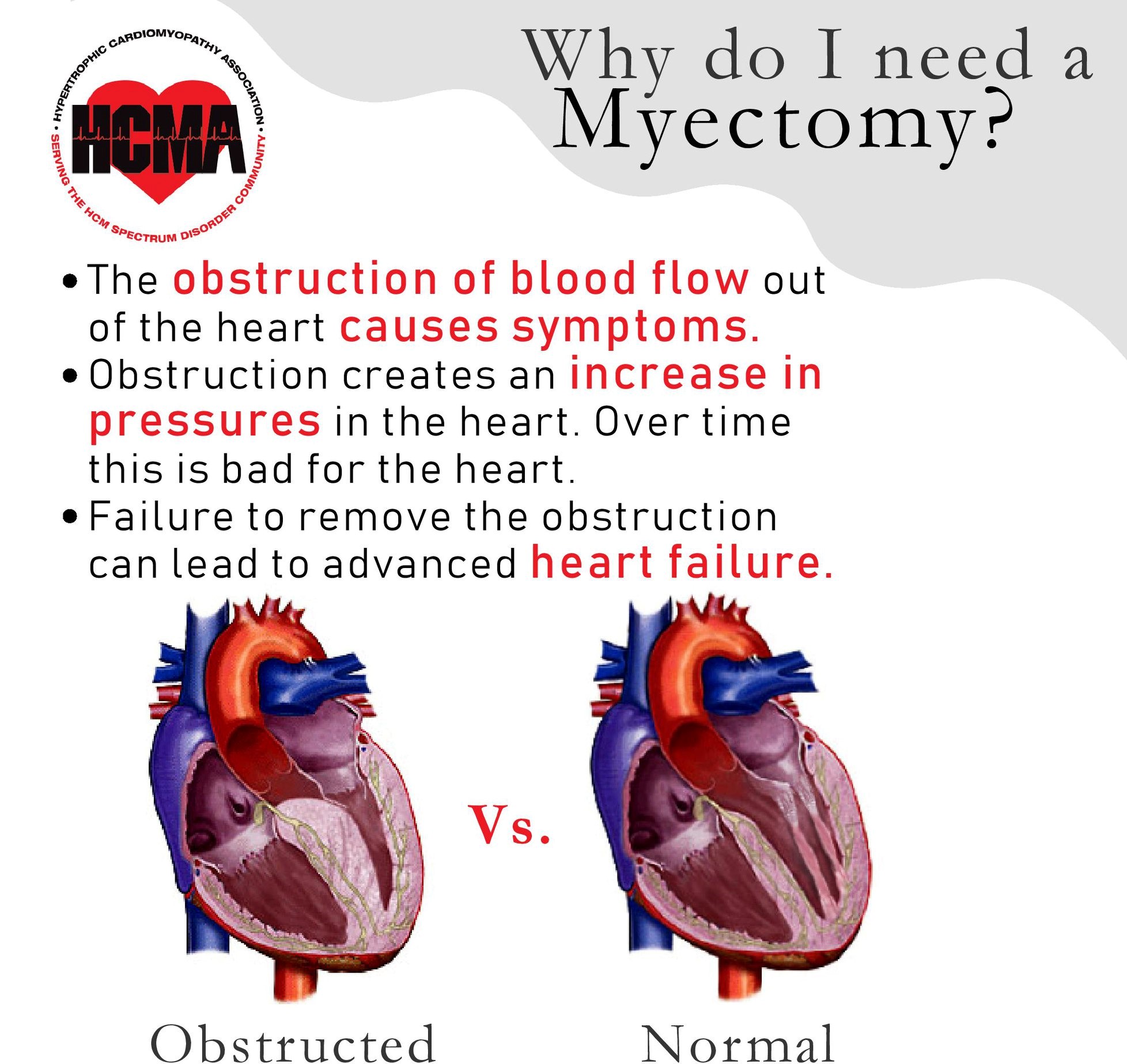
Finding a surgical team
Data show that myectomy is the safest and most successful procedure for reducing obstruction. Choice of surgical centers is very important. Data show that both safety and success of myectomy are much better at high-volume centers that perform many myectomies regularly. This is sometimes a difficult choice for patients because most of us do not travel for medical care. Besides, local surgeons may seem highly competent. But myectomy is a challenging procedure for surgeons. Having a surgical team that performs myectomy routinely makes a big difference.
Testing before surgery
Most centers will perform their own testing. They may repeat tests that have already been performed. They want particular information and they need confidence in what they are seeing. But they will certainly want to see the test results from other doctors. Before the surgery, they will perform a detailed echocardiogram to determine heart function and septal wall thickness. They may also perform an MRI, both to get more precise information and to assess how well your mitral valve is working. If you have an ICD or pacemaker, they will query them for data. A pre-surgical cardiac catheterization is normal, so that the surgeon can have good, recent information about your heart. The catheterization will tell the surgeon whether there are other problems that need to be addressed while your chest is open. Blocked arteries are a primary example. They will also perform blood tests and chest x-rays. You will have an appointment to get specific instructions about the surgery, further testing, and what to expect after the procedure. Usually you will be able to talk with your surgeon and anesthesiologist during the pre-surgical appointments. Centers can usually schedule things so that all the tests and appointments are done during the same trip as the procedure.
Surgical procedure
A typical myectomy lasts from 3-6 hours. Your anesthesiologist will make sure that you are anesthetized throughout the procedure. A 6-8 inch incision will be made down the center of your chest to divide the sternum (breastbone) and provide direct access to the heart. A cardiopulmonary bypass (heart-lung machine) will be used to take over the heart's normal function. This allows the surgeon to work on a heart that is not moving. The machine helps protect your other organs while your heart is temporarily stopped. Blood will run through the machine which helps exchange oxygen and CO2. This blood is then pumped back into the body.
The surgeon will make an incision into your aorta so they can access the thickened heart muscle through the aortic valve. This means that they do not have to cut through heart muscle to get to the septum. They will then remove tissue from the septum. The amount of tissue removed is often guided by performing a transesophageal echocardiogram in the operating room. They will also perform any other repairs that are needed. In HCM patients this may mean repairing or replacing the mitral valve, or repositioning the papillary muscles that open and close the valve. If other procedures are needed, like a coronary bypass, they will also be performed. The tissue in your septum will heal on its own without suturing. Once they have closed your aorta, your heart will be restarted and the bypass machine removed. Temporary pacing wires and a chest tube to drain fluids are placed before the sternum is closed. The skin and subcutaneous tissue are closed with internal, absorbable sutures.
Post-op hospitalization
After the procedure, you will be transferred to an ICU unit to be monitored for 1-2 days. This includes continuous heart, oxygen, and blood pressure monitoring, as well as frequent vital sign checks. You will then be transferred to a "step-down" unit in the hospital, and stay there for 3-5 days.
Time in the hospital can be longer or shorter depending on how fast you recover and what complications you experience. Usually they will get you out of bed and start you walking the first day you are in step-down. Walking means that you will be able to shower, which is usually quite welcome! Walking regularly in the hospital is very important to your recovery. Most patients cannot walk for long at first, and they walk slowly, but this improves every day.
If you need an ICD, it is usually implanted several days after your myectomy. Before you leave the hospital you will be given information about incision care, medication, activity, and lifestyle changes. You will be told about warning signs to watch for and who to call if you have these problems.
Safety and complications
Myectomies are safe procedures, and especially so at the high-volume centers. But all surgery has risks. Risks in myectomy include infection, arrhythmia, chest pain, heart attack, stroke, and death. High-volume centers have mortality risks from myectomy of about 0.4%.
Some problems are very common after myectomy. Atrial fibrillation (afib) is common after heart surgery, occurring in somewhere between about ⅓ and ½ of patients. Usually it goes away during your hospital stay. Having afib after heart surgery doesn't mean that you are likely to have afib after you recover. Pleural effusion (fluid in the sac around the lung) is fairly common, and usually goes away by itself. If you have a myectomy at a high-volume center, the teams there are very experienced in handling these and other complications. A very common complaint after myectomy is backache. This is a result of opening the rib cage. Some centers work with experienced medical massage therapists who can give significant relief of backache. The risk of death from myectomy is quite low (0.4%) at high-volume centers.
It is normal to have a new condition after myectomy called left bundle branch block (LBBB). This sounds upsetting to many patients if they are not expecting it. But by itself, LBBB is generally harmless. Myectomy involves removing enough tissue from the septum that electrical signals can no longer be conducted down the septum. Signals are instead conducted around the right side of the heart and back up through the septum. The left ventricle still gets the impulse that makes it contract. It just gets it with a slight delay, and this delay can be seen on the EKG. Knowing about this helps, because you can tell other doctors that you have LBBB as a result of surgery and that you're fine! LBBB is nothing to worry about unless you also have a right bundle branch block (RBBB). In that case, you will need a permanent pacemaker. Sometimes patients choose an alcohol septal ablation (ASA) to begin with, thinking that it is "less invasive" and so a better choice. But ASA normally causes RBBB. If you need a myectomy later, you will almost certainly be pacemaker-dependent.
Recovery at home
Full recovery from a myectomy usually takes about 6 to 8 weeks, but this can vary. Your doctor will tell you how soon you may drive. Most patients are able to drive after about 3-8 weeks. You should not drive or sit in the front seat of a car because if you are in a collision, the airbag will hit your chest with a lot of force. Since your sternum will not yet be healed, this can cause serious problems. You will receive guidelines from your doctor about how much weight you can pick up. Most surgeons will tell you not to lift more than 5-15 pounds.
Patients vary in how much help they need once they get home. Restrictions on lifting means that even if you feel up to it, you probably cannot do your own grocery shopping. Lifting your children or pets may also mean that you need help with those things. The same is true for housework. Most patients can prepare simple meals on their own. Unless you are fairly frail, you probably do not need nursing care.
Regular follow-up appointments with your regular cardiologist are important to see how well you are recovering. During these appointments, your medications may be adjusted. After you have recovered, you should see your cardiologist regularly. This is so even if you have no symptoms and feel fine. Most patients see their cardiologist at least twice a year. You should contact them if you start having symptoms that are new, more frequent, or more severe. Don't wait until your next appointment.
Myectomy is a treatment, not a cure
You will still have HCM after your myectomy. After all, it is a treatment for the symptoms of obstruction, not a cure for the disease itself. Your left ventricle will still be stiff, and most arrhythmias will still be there after your surgery. You may have a repaired or replaced valve, which needs proper care, or valve problems that were not severe enough to fix during myectomy. Even if you have no obstruction at all after myectomy, you will still have HCM! Most patients still need to take some heart medications after myectomy.
To maintain your health after surgery, it is important to follow the guidelines given by your doctor. Things that can make a difference are eating a heart-healthy diet with low sodium intake, and exercising regularly. It is important to treat high cholesterol and manage your blood pressure. If you are diabetic, managing your blood sugar is very important for your heart. Finally, weighing yourself daily to monitor for sudden weight gain is very important.. Sudden weight gain (more than 3 pounds in a day or 5 pounds in a week) may indicate heart failure. A key to success in treating heart failure is to treat it quickly.
Most people who have myectomies feel much better afterward, and are able to be more active.
Myectomy or alcohol septal ablation?
Myectomy is not recommended for patients who are poor risks for surgery. Generally this means people who are very frail because of age or other medical conditions. In those people, an ASA may be able to reduce their obstruction and relieve many of their symptoms. Because ASA requires very particular heart anatomy, it cannot be done in everyone. If you also need mitral valve repair or repositioning of the papillary muscles, they cannot be done during an ASA.